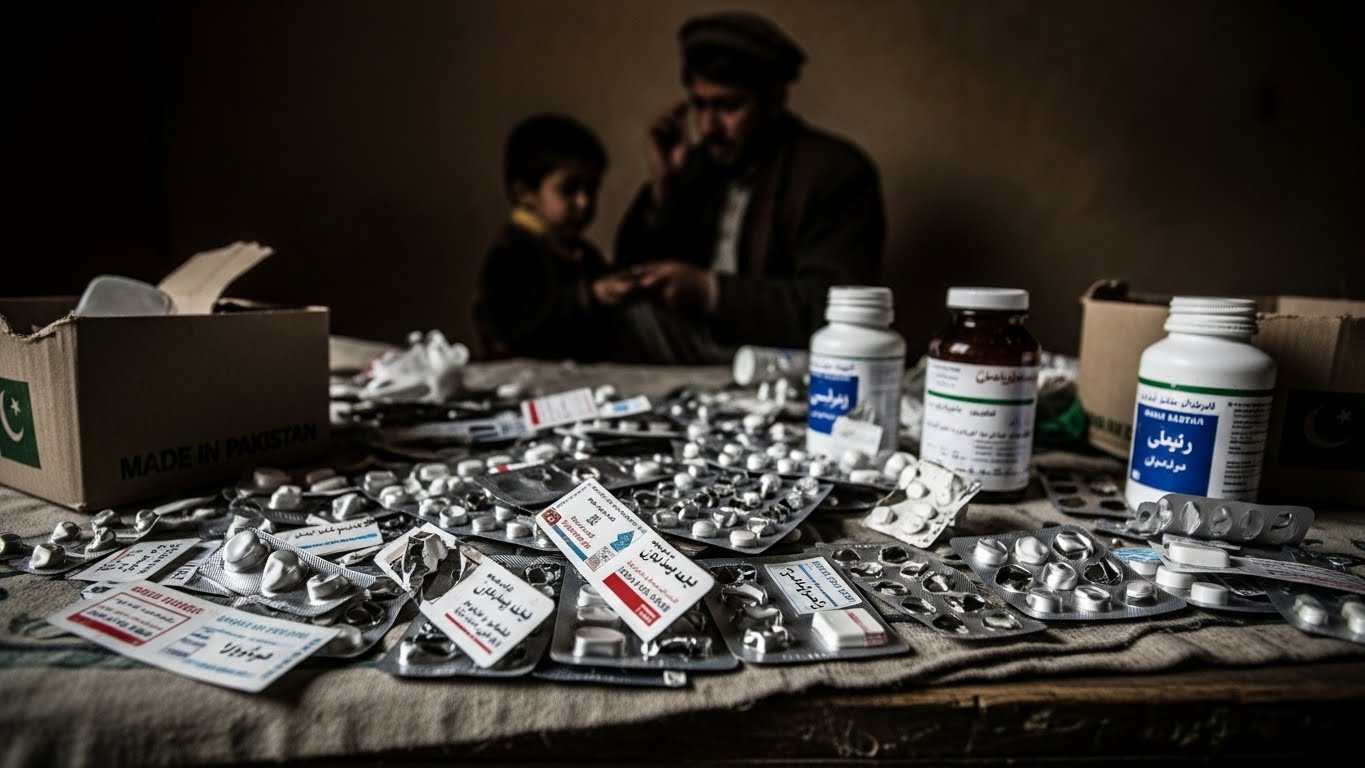
Afghanistan’s Medicine Crisis After Ban on Pakistani Imports
Access to affordable and reliable medicines is a fundamental pillar of public health, particularly in countries where local production is limited. Afghanistan has long depended on imported drugs to...
Access to affordable and reliable medicines is a fundamental pillar of public health, particularly in countries where local production is limited. Afghanistan has long depended on imported drugs to meet the healthcare needs of its population, with over 70% of essential medicines historically supplied by Pakistan. This supply chain not only ensured the availability of life-saving treatments across hospitals, clinics, and pharmacies but also maintained prices at levels accessible to ordinary citizens. The recent decision by the Taliban regime to ban Pakistani pharmaceutical imports has disrupted this critical network, raising concerns about shortages, rising costs, and wider implications for the country’s healthcare system.
The Taliban Ban and Its Implications
In November 2025, Abdul Ghani Baradar, deputy head of the Taliban regime and overseer of economic affairs, announced a complete ban on medicines from Pakistan. Afghan importers were given three months to settle outstanding debts with Pakistani suppliers and secure alternative sources. The justification cited was “poor quality” of Pakistani medicines.
Pakistan’s pharmaceutical industry, however, meets international quality standards and has supplied drugs to multiple countries reliably for decades. The abrupt ban left Afghan hospitals, clinics, and pharmacies struggling to adjust, threatening the consistent delivery of essential medicines.
Shortages and Rising Costs
The consequences of the ban have been immediate. In cities such as Herat, activists and pharmacy owners report that essential drugs—including insulin, heart medicines, and antibiotics—are becoming scarce. Hospitals have begun rationing supplies, putting patients with chronic illnesses at risk of treatment interruption.
Simultaneously, medicine prices have surged. Reports indicate that some essential drugs have increased by 50–100%, forcing families to choose between healthcare and basic necessities. This highlights how essential affordable Pakistani supply chains were to Afghan citizens.
Pakistan’s Role as a Reliable Supplier
Pakistan’s pharmaceutical industry has long been a trusted partner for Afghanistan. Medicines from Pakistan were:
- Affordable: Priced within reach of ordinary Afghan families.
- Reliable: Delivered in sufficient volumes to meet national demand.
- Accessible: Shared borders allowed fast and efficient transportation.
This dependable system allowed hospitals and pharmacies to maintain operations smoothly, even in rural areas. The abrupt severance disrupted decades of established logistics, straining Afghanistan’s health sector.
Afghanistan’s Alternatives: High Cost, Low Reliability
In response to the ban, the Taliban turned to India and other countries, reportedly signing a $100 million contract. But early reports show challenges:
- Indian medicines are significantly more expensive.
- Longer supply chains create delays.
- Some essential drugs remain unavailable, especially for chronic illnesses.
Smaller towns relying heavily on Pakistani supplies are particularly affected. There are also reports of expired or substandard medicines appearing in markets as demand outpaces stable supply.
The Human Cost
Ordinary Afghan families suffer most. Patients with diabetes, heart conditions, infections, and other chronic illnesses face interruptions in treatment. Rural communities with already poor access are seeing even more severe shortages.
With prices rising sharply, families that once relied on affordable Pakistani imports now face unaffordable healthcare costs. The disruption threatens both public health and economic stability.
Long-Term Risks for Afghan Healthcare
Without corrective action, the ban could cause lasting damage:
- Ongoing shortages may reduce hospital and clinic treatment capacity.
- Chronic illness management could worsen, increasing mortality.
- Households may face long-term economic strain.
- Trust in the healthcare system could erode as patients turn to unregulated markets.
With the loss of reliable Pakistani supplies, the healthcare system faces serious long-term challenges—especially in rural or underserved regions. The rising cost of imported medicines from distant suppliers deepens financial pressure on families, while substandard or expired products in the market worsen public health risks.
Conclusion
The Taliban’s decision to ban Pakistani medicine imports has exposed Afghanistan’s vulnerability in healthcare supply. Over 70% of Afghan medicines once came from Pakistan, ensuring affordability, reliability, and accessibility. The sudden disruption has caused shortages, rising prices, and life-threatening risks for patients.
While alternative suppliers may provide temporary relief, higher costs and logistical challenges make them far less effective. This crisis underscores the importance of stable, dependable, and cost-effective medicine supply chains for public health.
For millions of Afghan citizens, restoring access to essential medicines is not a matter of politics—it is a matter of life and death. Pakistan’s long-standing support demonstrated the value of practical and cooperative regional partnerships, highlighting what is at stake when such connections are severed.